Atrial fibrillation (AF) is the commonest arrhythmia carrying the burden of cerebral embolus (CE), systemic embolus (SE) and aggravation of heart failure (HF). The risk of emboli is increased in persona with risk factors detailed by CHADS-VASc (Congestive heart failure, Hypertension, Age more than 75 years, Diabetes, Stroke, Vascular disease, Age between 65 and 74 Years, Sex category) score of 2 or more.
Traditionally the risk of embolism with subsequent morbidity and mortality has been managed by Warfarin, a vitamin K antagonist (VKA). Warfarin has always plagued treating physicians with a narrow therapeutic index, drug interactions, and need for repeated monitoring of efficacy by the International Normalized Ratio (INR). The ROCKET AF trial reported that only 55% of patients in the warfarin arm were in the INR therapeutic range.
We now have the advantage of the novel oral anticoagulants (NOAC) that provide equal if not superior efficacy whilst reducing cerebral hemorrhage, fatal bleeds and possibly even mortality. The NOAC’s do not require constant monitoring and have antidotes available in the event of fatal bleeding. There has been a gradual acceptance of NOAC usage as seen by increased prescriptions of the new drugs. It is important to note that across the world oral anticoagulants (OAC) are underused in patients with AF.
The Veterans Administration reported 43% OAC (warfarin or dabigatran) use for new onset AF. The PINNACLE registry showed 45% OAC used in around 430,000 patients, while the GARFIELD-AF registry has reported 61% OAC use in 17,000 new AF patients from 30 countries. Hospital discharge data from 16 lakh admissions in 800 US hospitals revealed 46% OAC prescription in new onset AF patients.
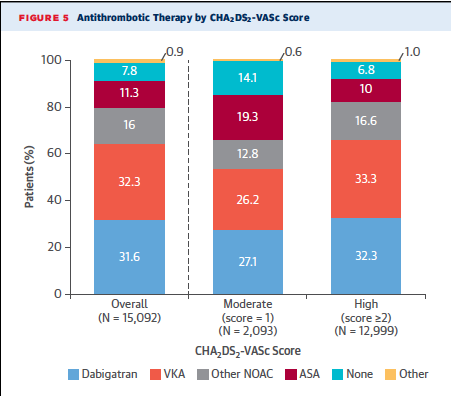
The GLORIA-AF (Global Registry on Long Term Oral Antithrombotic Treatment in Patients With Atrial Fibrillation) phase 2 registry however has reported a greater number of patients with AF on OAC. In the GLORIA-AF registry there were 53% patients with paroxysmal AF, 36% with persistent AF, and about 12% permanent AF patients. This registry describes OAC treatment in newly diagnosed patients all over the globe. The researchers report 80% compliance with OAC therapy; 48% on NOAC and 32% on VKA. Around 82% of patients with CHA2DS2-VASc score of 2 or more were on some form of OAC treatment.
Crucially, the most disturbing finding is that nearly 20% of AF patients are not on any stroke preventive therapy. Of these 10% had risk of bleeding but 10% of patients were on no or inferior treatment such as aspirin. It should be noted that OAC provides 64% reduction in risk of ischemic stroke and a 26% reduction in all cause mortality compared with control or placebo.
The only other registry reporting 80% OAC use has been the EurObservational Research Programme on Atrial Fibrillation) registry. The GLORIA-AF registry concludes that in newly diagnosed non-valvular AF patients there has been brisk adoption of NOAC treatment in Europe and North America, but quite a few patients get no treatment or were treated with aspirin, especially in Asia and North America.
These findings underscore the gaps in appropriate treatment of patients with AF at highest risk of stroke offer us challenges to understand the causes of the gaps and knowledge for improvement.