
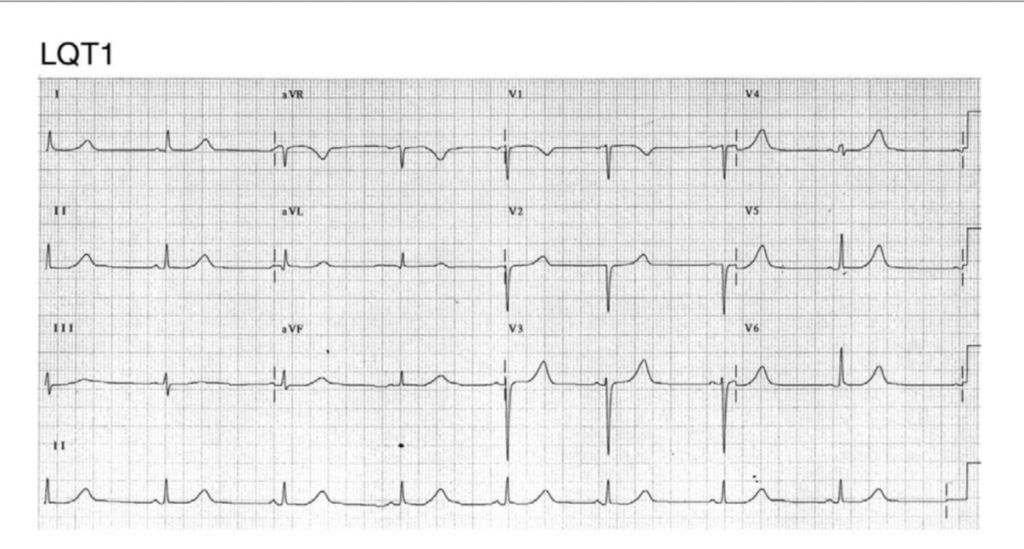
There is little data backing advice regarding congenital long QT syndrome (LQTS) and competitive sports. LQTS is a channelopathy characterised by abnormal QT interval prolongation on the ECG. LQTS defined by an abnormally prolonged QT interval (corrected QT interval >440 ms in men and >460 ms in women) with or without morphological abnormalities of T waves is a common cause of cardiac arrest. The prolonged QT interval due to decreased outward potassium currents or increased inward sodium currents predisposes to early after depolarizations and torsade de pointes ventricular tachycardia (VT). LQTS affects one in 2000 individuals. The annual rate of sudden cardiac death (SCD) is estimated to be between 0.33% and 0.9%, while the rate of syncope is 5%.
Twelve different genes are involved in inherited LQTS. The first 3 ; LQTS 1, LQTS 2, LQTS 3 account for > 90% of genotyped cases. Symptoms of seizure, syncope , or cardiac arrest usually appear at mean age of 12 years. Patients with LQTS 1 usually have symptoms with physical exercise and especially with swimming. Diving into water triggers the sympathetic system , while hitting cold water triggers the parasympathetic system due to apnea. The LQTS 3 is quite different in that VT is triggered while asleep or during rest. Emotional stress or ringing of a bell triggers VT in the LQTS 2 cohort. A corrected QT interval > 500 ms poses a high risk for a cardiac event. Beta blockers are indicated for all patients with syncope and also for asymptomatic with significant QT prolongation. Beta blockers are very effective in LQTS 1. The role of beta blockers in LQTS 3 is still not established, but symptomatic patients should receive beta blockers. Implantable cardioverter-defibrillator is indicated for secondary prevention of cardiac arrest and for patients with syncope despite beta blocker treatment.
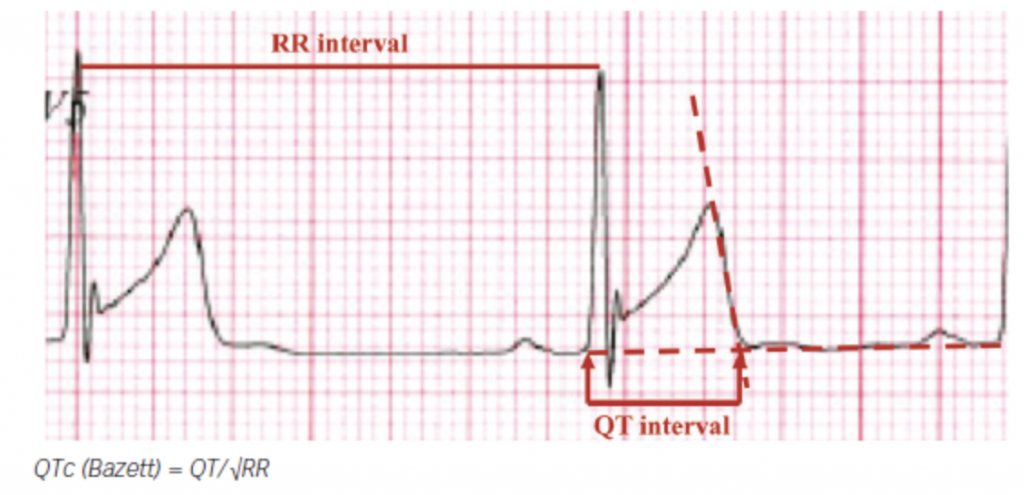
It should be borne in mind that the QT interval is longer in athletes than in non athletes because of the lower heart rate connected with training. But the corrected QT interval remains in the normal range albeit towards the upper limit. Corrected QT interval must be measured manually from the beginning of the QRS complex to the end of the T wave. The end of the T wave is defined as point where a tangent line to the steepest part of the descending portion of the T wave intercepts the isoelectric line. The QT interval is best measured in lead II or V5.
Athletes have a slow heart rate because of a higher vagal tone and this may make measurement of QT interval by the Bazett’s formula difficult. Bazett’s formula be comes inaccurate at heart rates < 40 BPM and >120 BPM. The ECG therefore in an athlete should be repeated after some aerobic exercise in order to get to a heart rate of 60 BPM, where no adjustment for heart rate is needed. It is important that acquired causes of QT lengthening such as medicines, hypokalaemia, and metabolic changes are excluded before diagnosing inherited LQTS.

The ECG of an endurance athlete should be repeated after 2-4 weeks before confirming the final measurement of the QT interval. Heart rate response on brisk standing is similar in patients with LQTS and normal people. But the QT interval in normals shortens by 40 ms whereas it increases by about 4 ms in the LQTS group. Genetic testing is recommended when there is strong clinical suspicion for LQTS based on clinical history, family history, and a corrected QT > 480 ms in an adult.
So what are the recommendations for competitive sports participation in patients with LQTS. The European guidelines of 2005 are the most restrictive. They recommend that LQTS (> 440 ms in men and > 460 ms in women) even without a documented major arrhythmia is a contraindication for any sport. The 2015 European guidelines for the prevention of sudden cardiac death however recommend avoidance of strenuous swimming especially in LQTS, with no mention off any other sport.
The 2015 American guidelines are less restrictive. The recommendation for the symptomatic athlete is that he or she should not compete. In the case of the asymptomatic patient with LQTS ( prolonged QT on ECG), a comprehensive evaluation of the athlete by a cardiologist (heart rhythm specialist) or a genetic cardiologist with sufficient experience with LQTS is mandatory. Treatment with beta blockers and adequate precautionary measures must be taken in the case of an asymptomatic patient of LQTS before permitting competitive sports, the athlete having been asymptomatic for the previous 3 months. The athlete and the family should be informed of the potential risks of participating in competitive sports.
The asymptomatic genotype positive/ phenotype negative athlete may participate in all competitive sports as long as adequate precautionary measures are taken. The athlete must avoid QT prolonging drugs, avoid dehydration, avoid training related heat exhaustion or heat stroke, and procure a personal automatic external defibrillator (AED). They must also ensure that an emergency action plan is in place with the school/ team officials.
There is some promising retrospective data available on LQTS and competitive sports.The signal from these studies is that serious cardiac events are uncommon in asymptomatic LQTS patients pursuing active competitive sports. In a group of 353 athletes with LQTS 63% decided not to participate. The remaining 130 patients ( or a little ore than one third) chose to continue participating in competitive sports. Most of them (87%) were treated with a beta blocker and 20 ( 15% ) had an ICD implanted. There was only one 9 year old boy who needed a DC shock (twice) but the little boy had stopped his beta blocker during these times. The overall rate of events per athlete year was 0.003 ( 1 event in 331 athlete years).The authors refer to the 36th Bethesda Conference that recommends that patients with either (1) symptoms, (2) corrected QT interval greater than 470 ms (males) or 480 ms (females), or (3) an implantable cardioverter-defibrillator should not participate in most sports. They also concluded that that there was a low rate of LQTS triggered cardiac events during sports ( Br J Sports Med 2012; 47:28-33)
Another retrospective study of 172 children with LQTS reported that almost 40% exercised in a recreational manner while the remainder indulged in competition. No syncopal events were reported during competition but 4 patients had syncope during recreational activity. There were no cardiac arrest or deaths reported during recreational or competitive exercise. These 2 studies are however limited by there retrospective nature, and small number of patients studied for short durations. Moreover the subjects were not involved with the highest cardiovascular demand ( J Am Heart Assoc 2017;6 (9): e005445). To draw firm conclusions from these 2 small studies would be premature.Both studies recognise that beta blockers are the foundation of treatment in LQTS, and should be considered also in carriers of a LQTS mutation who have normal QT interval. ICD implantation alongside beta blocker therapy is recommended in patients with previous cardiac arrest and also in patients with syncope and/or ventricular tachycardia while receiving adequate dose of beta blockers.
The American guidelines on LQTS and competitive sports that are less stringent than the European recommendations reflect an ethos where personal choice trumps over the state, while Europeans emphasise the role of the state overriding individual choice. The Europeans for a change are more conservative than the Americans.
A comprehensive screening program is not possible in m most countries due to constraints on financial resources and personnel. In the UK, the British Lawn Tennis Association, Premiership football and rugby league, and the national swimming and boxing squads have a self financed mandatory pre participation screening programmes of history, physical examination, 12 lead ECG and echocardiography in place. A British study reported the prevalence of prolonged corrected QT in elite athletes as 0.4%. The authors concluded that a corrected QT of >500 ms is highly suggestive of LQTS, while a corrected QT <500 ms in the absence of symptoms or familial disease was unlikely to represent LQTS in elite athletes. The diagnosis of congenital LQTS was based on the triad of prolonged QT interval, polymorphic VT or unheralded syncope and a family history of sudden cardiac death or LQTS ( European Heart Journal 2007;28:2944-2949).
In the US the advice on risk stratification is sought from the physician, after which the athlete is responsible for the final decision. The school/team officials also need to agree, of course, because in the event of an emergency they who will need to perform the required emergency procedure.This may explain the difference in the approach of Americans versus Europeans regarding LQTS and competitive esports. As usual, in India, there is little to go by. One may assume that the European restrictive protocol of forbidding competitive sports completely would be more aligned with the Indian mind set. Convincing an Indian parent of allowing her 10 year old child with LQTS to participate in an inter-school race would be near impossible. Add to that the cost of purchasing an automatic external defibrillator. Hence the current European guidelines (2005) recommending that patients with LQTS should be excluded from any competitive sports should be the mantra to be followed in India. The European recommendation seems both prudent and safer for now .
