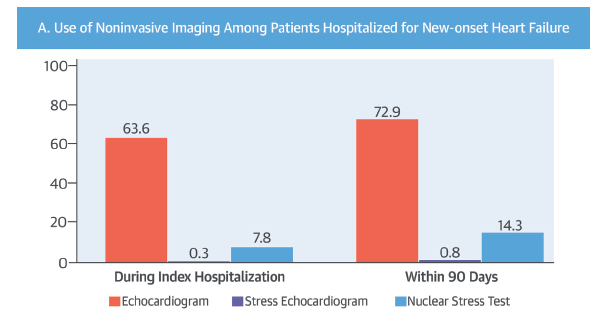
 A recent report in JACC (2016;68:450) provides the stunning realisation that of more than 67,000 patients admitted with heart failure in the USA, less than half a percent of patients underwent stress echocardiography to pick up coronary artery disease (CAD) as the underlying cause despite the fact that 50% to 60% of heart failure patients have CAD as the underlying triggering factor. Astoundingly more than 80% of patients did not undergo any form of testing for ischemic heart disease.
A recent report in JACC (2016;68:450) provides the stunning realisation that of more than 67,000 patients admitted with heart failure in the USA, less than half a percent of patients underwent stress echocardiography to pick up coronary artery disease (CAD) as the underlying cause despite the fact that 50% to 60% of heart failure patients have CAD as the underlying triggering factor. Astoundingly more than 80% of patients did not undergo any form of testing for ischemic heart disease.
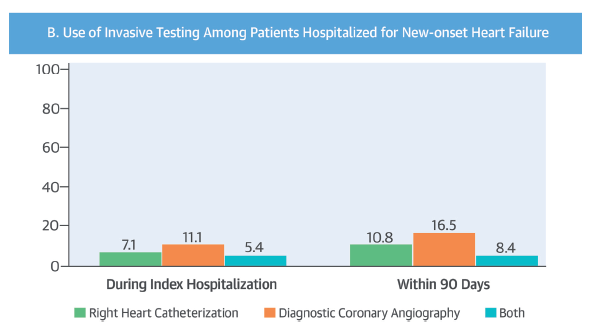
Only 11% of this large cohort of heart failure patients had invasive coronary angiography and just about 2% of patients had a revasularisation procedure during index hospitalisation. Less than 5% patients of heart failure underwent coronary bypass surgery or percutaneous coronary intervention.
The figures reported are startling as they come from the US, which traditionally follows the most aggressive treatment protocols in heart disease. The situation in India is worse. A middle aged obese lady sought consultation for her breathlessness and easy fatigabilty around 5 months ago, she was found to have poor left ventricular systolic dysfunction with an ejection fraction of 20-22% accompanied by moderately severe mitral regurgitation. I put her on a diuretic, angiotensin converting enzyme inhibitor, beta blocker, ivabradine and a statin. I advised her coronary angiography in order to figure whether CAD was the underlying cause albeit the fact that she had global hypokinesia. The patient achieved considerable relief in her symptoms and returned for advice after 5 months, but still undecided on coronary angiography. She demurred too on CT coronary angiography.
Heart failure is a real and massive burden on health care. More than 900,000 patients are diagnosed with new onset heart failure in the US alone. We currently do not have numbers from India. Heart failure is the only cardiovascular disease for which mortality and hospitalisation have worsened in the last 25 years.The prevalence of CAD is high both in systolic and diastolic heart failure. Ischemic CAD has become the number one cause for heart failure, toppling hypertension and valvular heart disease. Crucially, CAD may be treated or its progression delayed by suitable treatment. The STICH randomised trial demonstrated that over a follow up of 10 years CABG reduced mortality and improved quality of life when compared to optimal medical therapy. The STICH trial was published this year.
The retrospective analysis of more than 67000 patients of new onset heart failure concluded that there was severe underutilisation of assessment of ischemic heart disease. Another observational study involving 37000 patients also recorded marked underutilisation of stress testing in patients of heart failure (only one third of patients) in spite of the 2a indication ticked by the 2013 AHA/ACC guidelines for heart failure management.
In the OPTIMISE-HF study, coronary angiography during index hospitalisation resulted in significant reduction of mortality 60-90 days post discharge and increased usage of aspirin,statin and myocardial revasularisation. A substantial number of patients will have improvement in their left ventricle function with optimal medical therapy and there is always the potential of less resource utilisation because of dismissed emergency visits in the future.
Surprisingly almost one third of patients of new onset heart failure did not even gave a simple 2-dimensional echocardiography done. To miss transthoracic echocardiography in a hospitalised patient of heart failure should be considered criminal neglect.
It is important for the clinician to remember that although one cannot cure CAD, one can ameliorate symptoms and prevent comorbidities by providing appropriate treatment subsequent to confirming stenosed coronary arteries. We in India cannot echo the amazing gaps in US medical care as revealed in this study.