Elective percutaneous coronary intervention (PCI) has always included at least an overnight stay due to fears of acute complications such as myocardial infarction, bleeding or vascular complications. Over the years interventional cardiologists have acquired greater confidence with improved hardware and better percutaneous techniques whilst doing PCI procedures. The risks of major adverse events have gradually been shrinking and are actually quite low. Most major adverse events occur within 6 hours of PCI. A same day discharge (SDD) protocol has gradually emerged after single center randomized and observational SDD experience. Overnight stay remains standard practice after a PCI.
A meta analysis collected data from almost 13,000 patients undergoing PCI. The study included 7 randomized trials (2738 patients) and 30 observational studies (10,065 patients). Clinical outcomes consisted of myocardial infarction, death, target lesion revascularization (TLR) and majority of patients suffered from stable angina.
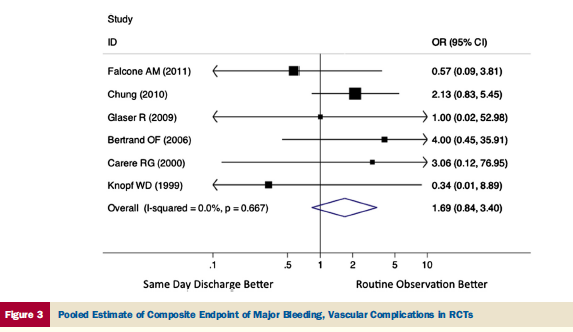
Vascular access in the randomized trials was predominantly radial (61 %), while it was femoral in the observational studies (71%). There was no difference in clinical outcomes between SDD patients and the routine observational cohort with regard to death/MI/target lesion revascularization. There was also no difference in bleeding /vascularization complications. Similarly there were no differences in the observational trials. The researchers concluded that in selected patients of stable angina undergoing elective PCI, same day discharge appeared to be as safe as routine overnight observation. There was no significant difference in Death, MI, TLR, readmission, stroke, major bleeding, vascular complications or minor bleeds. Nearly 28 % patients in the randomised and observational cohorts had multi vessel disease.
European centers have pioneered SDD by using the radial artery approach and avoiding use of GP IIb/IIIa inhibitors. Patients with comorbidities like low left ventricle ejection fraction < 30% and those with chronic kidney disease were excluded.
Another group of investigators has reported today that safe clinical outcomes with SDD after PCI. Their conclusion is that available evidence supports the safety of SDD in selected patients after PCI. The authors have discussed that the most common causes of lawsuits against cardiologists in the USA involve failure to diagnose acute coronary syndrome and aortic dissection. Death during cardiac catheterization is the commonest lawsuit against interventional cardiologists. It is important to inform the patient and family in SDD of potential risks after discharge and a plan in case an emergency is encountered. Expected risks of a procedure do not equate to malpractice.
Length of stay after PCI has steadily decreased because of advancements in pharmacology, technique, and technology. Same day discharge brings cheer to the patient and cuts down cost substantially for the hospital. It is estimated that if half of patients undergoing were discharged the same day there would be savings to the tune of $500 million per year. Medicare reimbursements for SDD following PCI are $9624 or Rupees 6 lakhs approximately (single stent) and $14,841 or Rupees 9.4 lakh respectively (two stents) in the USA, substantially greater than the cost in the most expensive corporate hospital in India. The cost provided here is not of overnight stay but of same day discharge and should be food for thought for health regulators in India.